Happy Holidays!
Happy Holidays. Wishing you every happiness this holiday season and throughout the coming year!

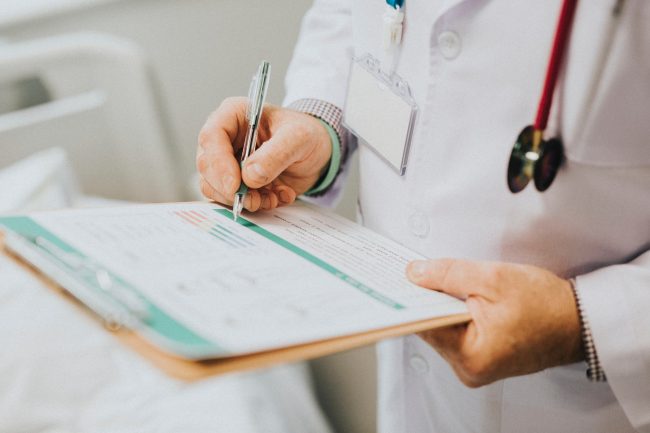
Telemedicine Improves Outcomes, Saves Money
Recent studies have shown that telemedicine can yield significant savings for group health plans and covered employees – but only if the employees actually use it.
While telemedicine has penetrated the ranks of large employers (96% say they make it available to their employees), 20% of employers say that less than one-tenth of their workers actually use it.Read More
60 Minutes – The Rockford File
60 Minutes: The problem with prescription drug prices
“Every company can make profits, but this is profiteering. This is gouging.”
On Sunday night, 60 Minutes covered what one city did to fight back against high drug prices by exposing an increasing corrupt drug supply chain. Continue the conversation with Tom Emerick, industry-leading consultant for Walmart, Burger King, and BP, May 15th to see how this type of supply chain corruption affects your business and what you can do about it.
Tout Tax Benefits of Long-term Disability Insurance to Your Staff
One of the most overlooked and undervalued employee benefits is long-term disability insurance. Often, even if the employer offers to cover the low premium, employees don’t sign up.
They think they won’t become disabled or need income replacement, despite some startling statistics: that about 25% of 20-year-olds will become disabled, even if temporarily, before they reach retirement.Read More
New Rules Lay Down Law for Group Plans in 2019
In the final rules that the Centers for Medicare and Medicaid Services released for 2019, it also covered annual cost-sharing limits for group plans, rules on SHOP exchanges, and grandfathered plans, among other items we’ve covered earlier.
Here we break down some of the focuses of the 2019 rules:Read More
Maximum Family HSA Contribution Reduced for 2018
One of the unintended consequences of the tax bill that was signed into law by President Trump in December was a change to the HSA contribution limits for 2018, and action needs to be taken for some participants immediately.
As a result of the new tax law, the IRS announced in March that the maximum family contribution to a health savings account for 2018 is being reduced by $50 (from $6,900 to $6,850).Read More